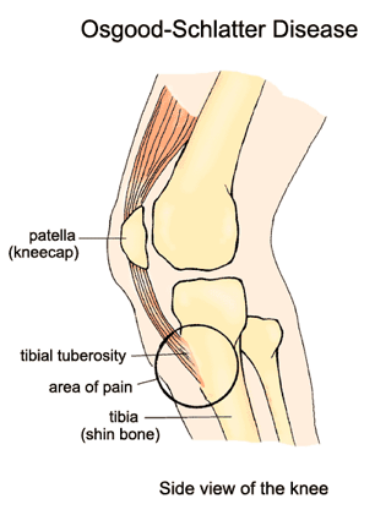
Osgood-Schlatter disease is a painful enlargement of the bump on the top of the shin bone (tibia) just below the knee. This bump is called the tibial tuberosity. The tendon that attaches the kneecap to the shin bone attaches at the tibial tuberosity. There is a growth plate in this region that is soft bone. Osgood-Schlatter disease is most often seen in children between the ages of 10 and 15 and usually appears during a period of rapid growth where this soft bone can become inflamed and swollen.
How does Osgood-Schlatter disease occur?
Osgood-Schlatter disease is caused by a loading overuse of the knee in normal childhood and sporting activities. It is possible that muscles are too tight in the front of the thigh, pulling on the growth plate and causing pain.
What are the knee symptoms?
Your child will complain of a painful bump below the kneecap. You or your child may notice a soft bony enlargement at the top of the shin bone. The pain will most times be worse AFTER activity once the body has cooled down. If pain develops DURING activity and exercise, that would indicate an advanced state of injury.
How is it diagnosed?
Diagnosis can in most cases be made after a physical examination. Your child may need an x-ray although this is often not required. X-rays may be required if no improvement is made within 4-6 weeks and there is a suspicion of plate fracture or loose body fragments.
How is Osgood-Schlatter disease treated?
Your child will need to reduce unnecessary activity. In severe cases total rest may be required. In most cases we can avoid total rest and maintain some form of activity. Ice packs will help reduce inflammation with proper application. Orthotic correction of poor foot and walking mechanics can greatly impact the function of the knee. This may help reduce symptoms.
How long will the effects last?
As your child gets older and past the rapid growth stage, symptoms of Osgood-Schlatter disease go away and there is usually no longer a problem. If left untreated during the growth phase, a permanently enlarged bump on the tibia may persist. It commonly takes anywhere from 6 weeks to 6 months from the start of the symptoms for pain reduction depending on treatment effect and the compliance of the child. The best way to avoid the pain of Osgood-Schlatter disease is to maintain the flexibility of the anterior thigh muscles known as the quadriceps.
As the growth plate hardens post-adolescence, there will be a small bump of bone where the pain was. This is normal in adults. It is possible for your child to sometimes have pain in the area of the bump even after he or she is an adult. In rare cases, adults with persistent pain from bony fragments around the knee need to have the fragments surgically removed.
When can my child return to his or her normal activities?
Everyone recovers from an injury at a different rate. Return to your activity will be determined by how soon your child’s knee recovers, not by how many days or weeks it has been since the injury has occurred. In general, the longer your child has the symptoms the longer it may take to recover from, so it is always a good idea to get these injuries examined as soon as possible. The goal of rehabilitation is to return your child to normal activities as soon as is safely possible. If your child returns too soon he or she may worsen the injury.
Your child may safely return to his or her sports or activities when, starting from the top of the list and progressing to the end, each of the following is true:
- The injured knee can be fully straightened and bent without pain.
- Your child’s tibial tuberosity is no longer tender.
- Your child is able to jog straight ahead without limping.
- The knee and leg have regained normal strength compared to the uninjured knee and leg.
How can Osgood-Schlatter disease be prevented?
Osgood-Schlatter disease may be difficult to prevent. The most important thing to do is to have your child limit activity as soon as he or she notices the painful bump on the top of the shin bone. We have found that consistent stretching of the front muscles of the thigh helps reduce or prevent its onset.

Dr. Sami Karam, Osteopath
I’ve been a qualified Osteopath since 2004. I’ve been playing football ever since I could remember and I have a passion for it. I’ve played at the highest level in the NSW State League at both Youth and Senior levels, and have also been Head Physician at numerous State League Clubs. I’ve travelled internationally and consulted with Sports academies in Barcelona and Italy. I have a special interest in Strength and Conditioning for footballers, as I believe it gives them an edge in their physical competition. My passion involves bringing all of this knowledge into every single treatment that I provide for all athletes. If you feel that I can help you and want to reach out to me, contact me.